Research Institute
Department of Artificial Organs
Member
| Director | Tomohiro Nishinaka |
|---|---|
| Visiting Director | Eisuke Tatsumi |
| Laboratory Chief | Tomonori Tsukiya Toshihide Mizuno Akihide Umeki |
| Research fellow | Hiroaki Aizawa |
| Researcher | Kyoko Shioya |
| Research assistant | Yukihide Kakuta Maki Nakanishi Ariyoshi Nakamura Sora Mimaki |
Research
The mission of the Department of Artificial Organs is to contribute to the conquest of cardiovascular diseases through the practical application of medical devices such as ECMO systems and ventricular assist devices (VADs) for the treatment of severe heart failure and respiratory failure. We are conducting medical and engineering research on the development of devices, their effects on patients and optimal control methods. Currently, several device development projects are underway in collaboration with companies. In addition, we are developing non-clinical test facilities, which are essential for improving the quality of medical treatment using these devices.

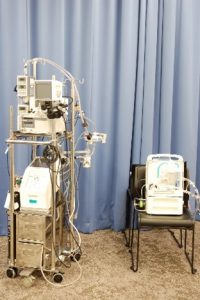

Left : Durable Centrifugal Pump for Mechanical Circulatory Support (BIOFLOAT®NCVC®)
Center : Durable ECMO System and Portable ECMO System
Right : Mechanical Mock Circulation System for Bench Testing
Publication
Akiyama D, et al. Preclinical biocompatibility study of ultra-compact durable ECMO system in chronic animal experiments for 2 weeks. Journal of Artificial Organs. 2020;23(4):335-341. doi: 10.1007/s10047-020-01180-1.
Shimamura J, et al. Miniaturized centrifugal ventricular assist device for bridge to decision: Preclinical chronic study in a bovine model. Artificial Organs. 2019;43(9):821-827. https://doi.org/10.1111/aor.13459
last updated : 2025/04/22
